Effective interprofessional relationships are essential for patient safety and lead to higher quality patient care. Despite this, there are obstacles in how we prepare health care professionals to care for their patients as part of an effective team. Barriers include lack of education about other health professional roles (like nurses, doctors, therapists, pharmacists, social workers, chaplains, etc.) and missed opportunities for collaboration and communication with these team members. Learners need experience working with and communicating as teams to understand the roles and contributions of other health disciplines. The current pandemic also highlights the need for health care professionals to work as teams to acquire new skills and creative solutions that overcome physical distancing barriers and address the social isolation of patients with chronic and serious illness and their families. There is no better time than now for health science faculty to help our students learn adaptation skills by finding new approaches to clinical learning that overcome the isolation and distancing of students, faculty, and patients alike.
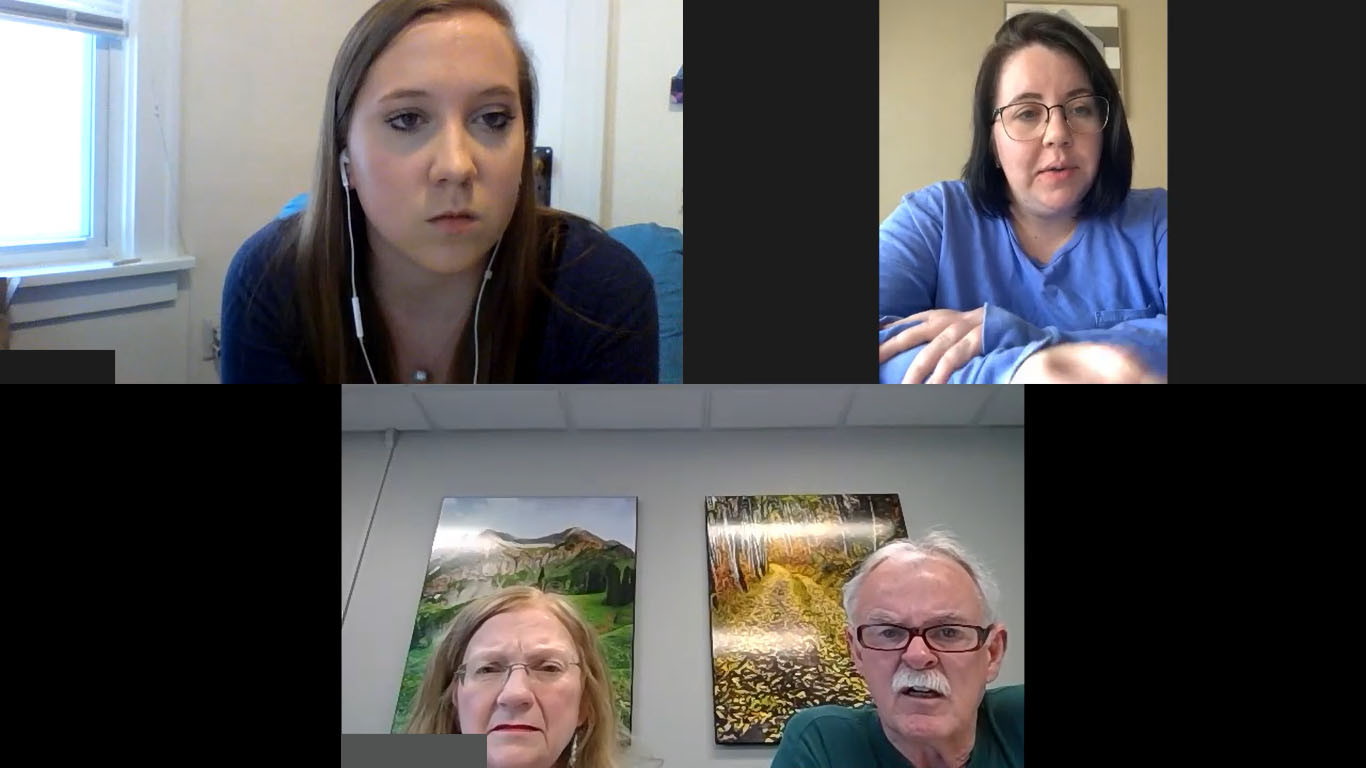
While online education offers flexibility and self-paced instruction, it often leaves students craving personal connections — especially during a pandemic. Providing real-time virtual opportunities that engage and connect students who now find themselves in different areas of the country and with very different schedules can be challenging. Virtual Interprofessional Simulation (VISion) is an experiential learning activity that overcomes physical distancing barriers, promoting collaboration and team-based competency development while connecting learners in meaningful relationships with peers and patients. Using a live video-based web conferencing platform, students interact with actors and students from other programs like occupational therapy and dentistry in virtual simulations. This provides them with the human connection they need while practicing how to effectively work in interprofessional teams to address the needs of the patient (played by the actor[s]).
For many programs, simulations are solely conducted in person with specialized equipment and environments created to enhance realism. In the past, educators and students have shared concerns that conducting simulations outside of these facilities built specifically to conduct simulations would be too limiting and likely unrealistic. We have seen that after educators and students participate in VISion or observe these web-based simulations, their concerns are assuaged.
We conducted a pilot study of the VISion strategy in an interprofessional palliative care course with health science students from seven programs (undergraduate and graduate nursing, social work, medicine, occupational therapy, physical therapy, and pharmacy). While at first these simulated team meetings started out with uncertainty, often with a long awkward silence while students hesitated and wondered which team member was going to take the lead, soon the students were clamoring at the chance to collaborate and share their unique roles and perspectives on the case. They quickly adapted to the etiquette of participating in a web conference, recognizing social cues and breaks in conversation by staying attentive to their video feed and muting/unmuting their microphones. One student commented, “I was scared and sort of unprepared for sim(ulation) because I didn’t know what to expect. But as nerve-racking as the simulations were, they definitely helped me to grow and understand….”
We used a palliative care scenario for the pilot as it is an ideal platform for demonstrating interprofessional dynamics requiring a multidisciplinary approach to care. Students developed a plan of care for ‘Hazel’, an elderly female suffering from recurrent symptoms of her chronic conditions and visited with her family during two phases of care. Students were first exposed to Hazel’s case midway through the semester, when she was hospitalized for an acute exacerbation of her heart failure, and later revisited Hazel’s case at the end of the semester, when her condition deteriorated and she was placed on home hospice. The pilot confirmed VISion is an effective experiential learning approach that enhanced students’ understanding of interprofessional roles, increased their confidence in team communication, and strengthened their performance of collaborative practice and patient-centered problem-solving.
One great benefit of VISion is its flexibility — students can participate in the simulation from anywhere with a wi-fi connection and mobile device with a camera. During the pilot, students were able to participate from cars, hospital on-call rooms, dormitories, and classrooms in different time zones simultaneously. The students were able to build rapport and productive relationships with one another, stating they felt more connected to faculty and the university as a result of the live face-to-face interactions that are rare with other distance learning techniques like discussion boards or virtual reality. Participating in VISion through a video web-conferencing platform requires students to consider their non-verbal characteristics (posture, eye contact, facial expressions, etc.), in addition to their communications skills, and the disposition of other team members and the standardized patients (actors) they are communicating with. This aspect of video-based virtual simulation becomes particularly important in developing the essential skills of relationship building, collaboration, and facilitating difficult conversations with patients and family members.
A student reflected on the VISion experiences saying, “I found the simulations to be the most valuable aspect in this course. I don’t feel that we have enough exposure to working in interprofessional teams and seeing how that benefits the patient. Simulation gave me the insight to working with other professions and seeing how I can develop more.”
We anticipate that country will see a second wave of COVID-19 coming during the fall semester. As educators prepare for the impacts of social distancing and directed health measures, which could limit student access to traditional clinical learning environments, planning of virtual activities needs to begin now. We can overcome physical distancing barriers to interprofessional education by working together to develop robust experiential learning activities that foster a spirit of teamwork and collaboration among all health professionals. In spite of nationwide program disruptions, integrating VISion as a web-based alternative for interprofessional clinical learning is one way to ensure newly licensed generalist practitioners of every profession grasp the value of each health care team member and the importance of collaboration and effective communication to provide the best, safest patient care possible.
We have learned a lot over the last three years of implementing this approach at Creighton University, including similar findings in other courses and the importance of adherence to simulation best practices. We’ve developed a number of tips for success and resources for VISion to support faculty adopting this strategy.